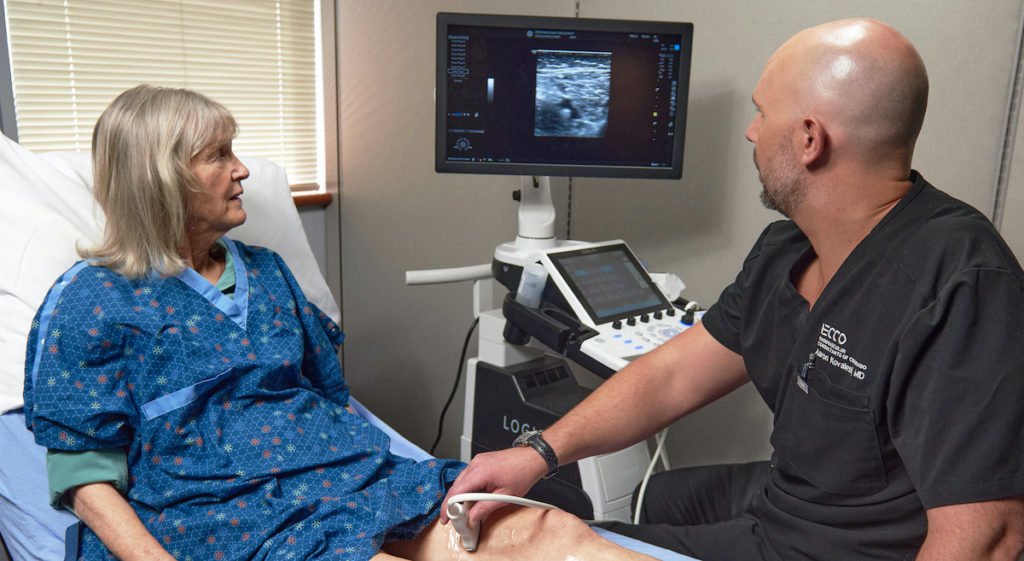
Studies show that one in three diabetics over the age of fifty have Peripheral Artery Disease, or PAD. And those with diabetic neuropathy run the risk of missing PAD symptoms if left unchecked and unscreened.
If diabetes goes uncontrolled, blood sugar levels increase. Increased blood sugar can narrow the arterial walls with accumulation of fats, cholesterol, and other substances. In other words, atherosclerosis. This results in poor circulation to the feet and legs which can further irritate already damaged nerves in patients with diabetic neuropathy.
Diabetic Neuropathy Often Masks PAD
Neuropathy, or nerve damage (typically in legs), often masks PAD symptoms. The most common initial symptoms are calf pain during walking and early leg muscle fatigue. However, other symptoms include a cold sensation in your lower leg or foot, especially when compared with the other side. Lastly, symptoms can also include sores on your toes and feet, or legs that won’t heal.
In other words, damaged nerves are unable to send the appropriate signals to the brain letting the patient know they are having issues in their legs. This can lead to delayed diagnosis and progression of PAD. Often, diabetics with neuropathy are not screened for PAD as they express no symptoms commonly associated with PAD.
Endovascular Treatment of PAD
Specialized, minimally invasive arterial interventions can help advanced cases of PAD. Depending on the case and its severity, therapies may include:
- Balloon Angioplasty: This therapy uses a balloon to open a narrowing or blockage in an artery. Performed with a specialized catheter, this technique uses an elongated balloon, or its tip, that inflates upon entry.
- Atherectomy: This procedure removes plaque buildup in arteries. This procedure uses specialized catheters that have a laser, or grinding functionality, to clear any blockage in the targeted artery.
- Stent Placement: If angioplasty or atherectomy aren’t successful in restoring flow through an artery, a stent, or a tube made of metal wire, keeps the vessel open. This is a permanent implant.
Each procedure listed requires moderate sedation and minimal recovery time. Compared with vascular surgery, endovascular interventions avoid the need for general anesthesia. That means patients have a shorter recovery period and fewer complications, making this a better option for frail patients who cannot undergo anesthesia and surgery.
Untreated PAD Consequences and How to Avoid Them
Individuals with diabetes have a significant risk of gangrenous wound development on the toes and feet which can lead to amputation if left untreated. It is critical to understand the connection between PAD and diabetes. Knowledge of the connection can help lower the risk of complications.
Education and early screening are key to preventing PAD in diabetics. At ECCO we strive to educate patients and the medical community about the increased risks associated with diabetic neuropathy and PAD.
In conclusion, if you are a diabetic and have neuropathy – talk to your primary care physician or podiatrist about PAD screening. Make your doctor aware of any additional risk factors such as high blood pressure, high cholesterol, obesity, coronary artery disease, and previous stroke.
The current recommendation is annual PAD screening for diabetics with neuropathy. Call ECCO and set up your screening today!